Coronaviruses are a large group of viruses that can cause illness in animals and humans. Some coronaviruses commonly circulate in the United States and usually cause upper respiratory symptoms such as cough or runny nose, although some can cause more serious illness. The 2019 novel (new) coronavirus causes the illness coronavirus disease 2019 (COVID-19).
The symptoms
People with COVID-19 have had a wide range of symptoms reported – ranging from mild symptoms to severe illness. Symptoms may appear 2-14 days after exposure to the virus. People with these symptoms may have COVID-19:
- Medical health history
- Fever or chills
- Cough
- Shortness of breath or difficulty breathing
- Fatigue
- Muscle or body aches
- Headache
- New loss of taste or smell
- Sore throat
- Congestion or runny nose
- Nausea or vomiting
- Diarrhea
Older adults and people who have severe underlying medical conditions like heart or lung disease or diabetes seem to be at higher risk for developing more serious complications from COVID-19 illness.
Testing
Learn more about the different types of tests and the steps involved.
Types of Tests
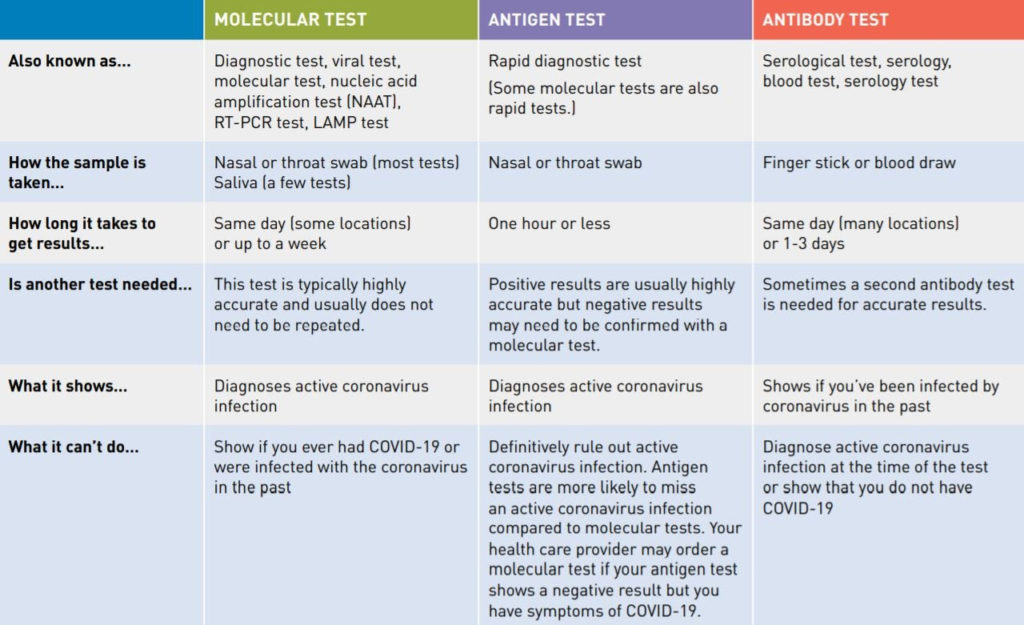
There are two different types of tests – diagnostic tests and antibody tests.
-
A diagnostic tests can show if you have an active coronavirus infection and should take steps to quarantine or isolate yourself from others. Currently there are two types of diagnostic tests which detect the virus – molecular tests, such as RT-PCR tests, that detect the virus’s genetic material, and antigen tests that detect specific proteins on the surface of the virus.
-
An antibody test looks for antibodies that are made by your immune system in response to a threat, such as a specific virus. Antibodies can help fight infections. Antibodies can take several days or weeks to develop after you have an infection and may stay in your blood for several weeks or more after recovery. Because of this, antibody tests should not be used to diagnose an active coronavirus infection. At this time researchers do not know if the presence of antibodies means that you are immune to the coronavirus in the future.